Pennsylvania GeriatricS Society
POLST NEWS |
POLST HAS A NEW WEBSITE |
The Pennsylvanian POLST Collaborative is announcing a new POLST website that increases accessibility to POLST information. To reach the new site, users can go to www.papolst.org. |
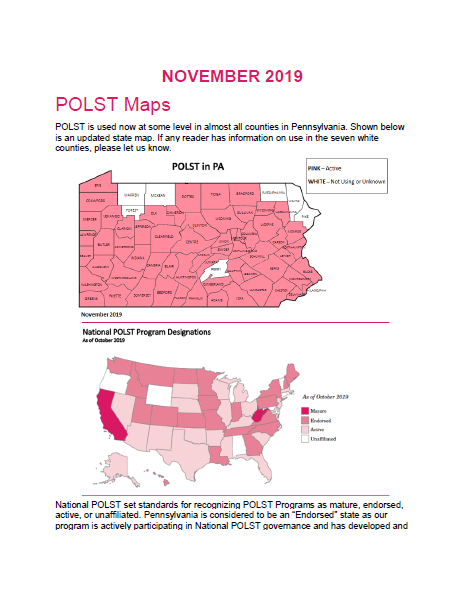
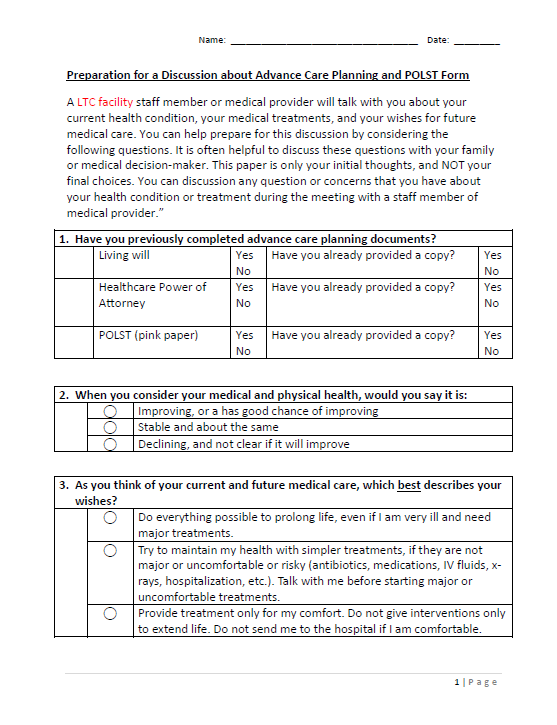
What Is POLST?The POLST process was created to translate a patient's specific goals for end-of-life care into a concise medical order that can follow the patient across all care settings. POLST directives are entirely voluntary and often developed through communication between a patient, their caregiver, and their physician following a terminal diagnosis. Directives typically include specifications about out-of-hospital do-not-resuscitate preferences, use of antibiotics, certain comfort measures, and other end-of-life considerations. Without these clear directions ensuring the patient's wishes are followed and the level of care desired by the patient is delivered – healthcare providers may be left with conflicting directions. POLST helps to eliminate that confusion. How Does POLST Differ from Advance Directives?POLST orders differ from advance directives in that POLST directives make clear an individual's wishes regarding treatment measures via a legal medical order that is applicable across all health care settings – applicable in emergency medical services, health care facilities, home care and hospice settings. Advance directives often only identify a surrogate health care decision-maker and lack specificity regarding a patient's end-of-life treatment preferences. Although POLST forms are currently available in Pennsylvania, these forms presently are not recognized by Pennsylvania law. SB 623 seeks to codify these orders and require that physicians, nurses, emergency medical technicians, and other medical professionals deliver care consistent with a patient's end-of-life preferences. |
POLST UPDATE - NOVEMBER 2019 |
UPCOMING EVENTS AND ADDITIONAL POLST RESOURCES
Please be aware of a new article published in the Journal of Palliative Medicine. The article reports on a cohort of Oregon decedents and among the trends noted are:
b.) Substantial increases in time from POLST completion to death; c.) Disproportionate increases in orders for more aggressive life-sustaining treatment. Based on these findings, the authors recommend testing new criteria for POLST completion in frail elders. To read or cite this article; Dana M. Zive, Valerie M. Jimenez, Erik K. Fromme, and Susan W. Tolle.Journal of Palliative Medicine, https://www.liebertpub.com/doi/10.1089/jpm.2018.0446. We have been informed that you can share the link to the article, post it, and reproduce as the Oregon POLST Program paid the fees for Open access. Some of you may be familiar with the research and writings of Dana Zive, MPH, who has recently served at the Director of the Oregon POLST Registry and Associate Director of the Center for Ethics in Health Care at OHSU. Sadly, Ms. Zive passed away suddenly this past September at the age of 42. |
NATIONAL POLST PARADIGM TALKING POINTS |


ADDITIONAL POLST RESOURCES |
About usThe Pennsylvania Geriatrics Society – Western Division is dedicated to improving the health and well-being of all older persons. It is a non-profit organization of physicians and other health care professionals committed to the provision of quality health care for older persons. | Contact usPennsylvania Geriatric Society - Western Division Chapter Administrator: Haley Thon | hthon@acms.org
|